- Understanding Low Blood Sugar
- Risks Associated with Hypoglycemia
- Diagnosing Hypoglycemia: A Comprehensive Approach
- The Importance of Regular Blood Sugar Monitoring
- Dietary Management’s Crucial Role in Blood Sugar Control
- Role of Medication in Managing Low Blood Sugar
- Exercise and Lifestyle Modifications for Managing Low Blood Sugar
- Recognizing a Hypoglycemic Emergency
Understanding Low Blood Sugar
Low blood sugar, medically known as hypoglycemia, is a condition that occurs when the concentration of glucose in your blood drops below normal levels.
Common Causes of Hypoglycemia
- Excessive insulin or oral diabetes medication
- Skipping meals or not eating enough carbohydrates
- Strenuous exercise without proper food intake
- Certain medical conditions like kidney disorders
Learn more about these causes here.
Symptoms of Low Blood Sugar
When blood sugar levels fall, symptoms may include dizziness, shaking, sweating, hunger, irritability, and confusion. Severe hypoglycemia can lead to loss of consciousness or seizures. Recognizing these signs and responding swiftly is crucial.

Understanding hypoglycemia and its triggers can help you manage your blood sugar levels and maintain your health.
Risks Associated with Hypoglycemia
When it comes to hypoglycemia, or low blood sugar, there are several risks you must be aware of. The immediate health risks include symptoms like shakiness, confusion, and even loss of consciousness. Without prompt treatment, severe hypoglycemia can be life-threatening.
Mayo Clinic provides an in-depth look into these immediate symptoms.
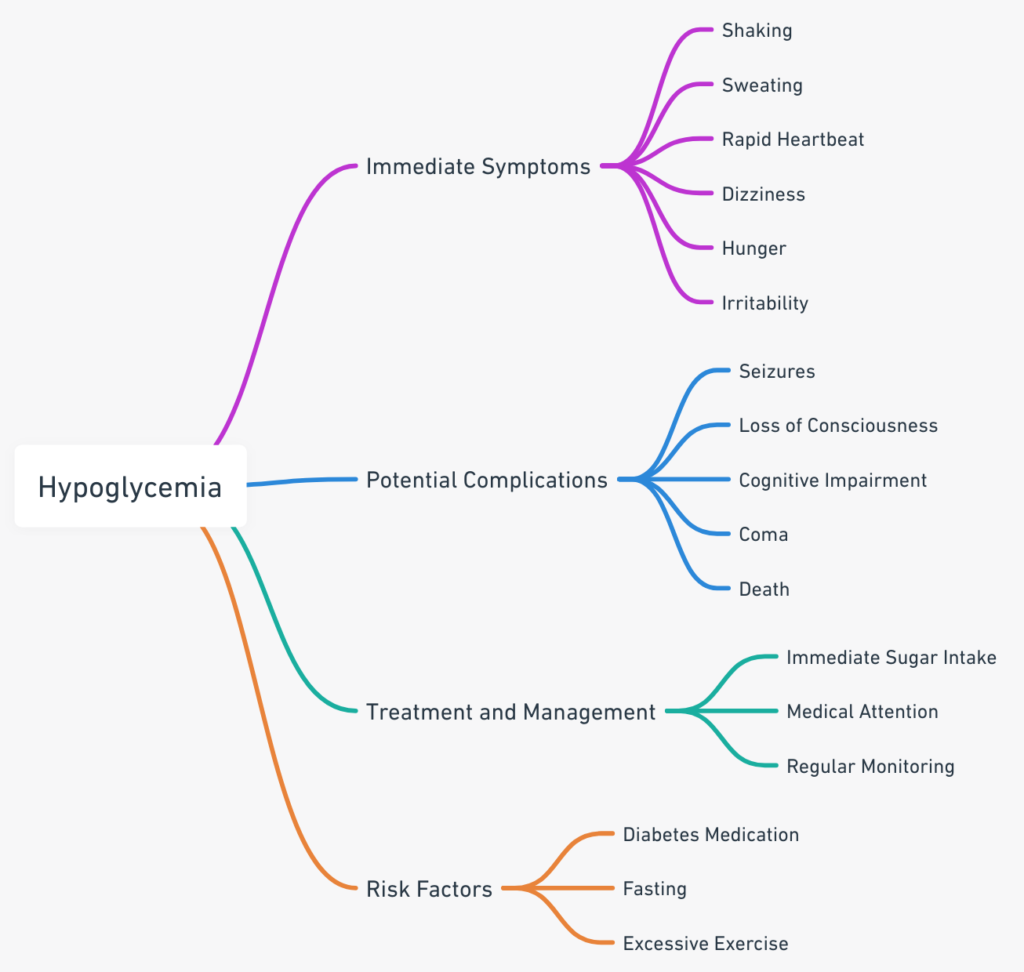
Long-term health complications can also ensue.
Repeated episodes of hypoglycemia can lead to cognitive impairment and cardiovascular disease, as explained by the National Institutes of Health.
Moreover, living with hypoglycemia can significantly affect your everyday life.
A constant need to monitor blood sugar levels can lead to anxiety and disrupt daily activities. Learning to manage hypoglycemia effectively is vital for maintaining your quality of life.
An informative guide from the Centers for Disease Control and Prevention can assist with this.
It’s imperative to understand these risks and learn how to manage your condition effectively to avoid these complications and live a healthier life.
Diagnosing Hypoglycemia: A Comprehensive Approach
Successfully diagnosing hypoglycemia requires a systematic method, combining physical examinations, thorough medical history reviews, and careful symptom assessment.
Medical and Physical Tests
Medical practitioners often apply the Whipple’s triad in diagnosing hypoglycemia. This involves the correlation of low glucose levels from lab tests with symptoms and their disappearance post-glucose normalization. Here, blood tests, insulin tests, and C-peptide tests are crucial.
The Role of Medical History
An exhaustive review of the patient’s medical history is equally important. It helps to identify any underlying conditions that may cause hypoglycemia, such as diabetes or pancreatic abnormalities. Additionally, it unveils any medication intake contributing to low blood sugar.
Reviewing Symptoms
Last but not least, symptom analysis is essential. Symptoms like sudden hunger, shaking, sweating, confusion, and blurred vision can all indicate hypoglycemia. However, these symptoms may overlap with other conditions, making a comprehensive diagnosis approach vital.
The Importance of Regular Blood Sugar Monitoring
Regular monitoring of blood glucose levels is crucial in managing low blood sugar. It helps you understand how your body reacts to certain foods, physical activity, medications, and stress, allowing you to make necessary adjustments to keep your blood sugar within a healthy range.
Types of Blood Glucose Meters
There are several types of blood glucose meters available, including traditional, continuous glucose monitors (CGMs), and flash glucose monitors. These devices differ in their features, cost, and convenience, but all provide valuable information about your blood glucose levels.
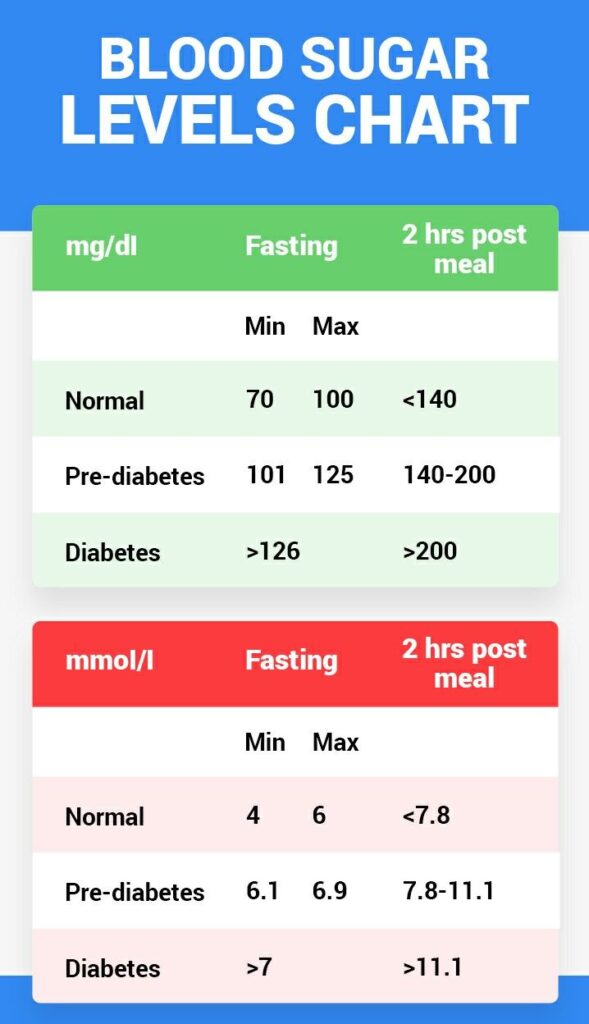
Interpreting Blood Glucose Results
To effectively manage low blood sugar, it’s essential to understand how to interpret your blood glucose results. Glucose levels can fluctuate throughout the day. By comparing your readings with the target ranges provided by your healthcare team, you can identify patterns and trends that may require adjustments in your treatment plan.
Dietary Management’s Crucial Role in Blood Sugar Control
Managing your diet is a powerful tool in controlling blood sugar levels. The types of food you consume, their portion sizes, and your meal timings significantly impact your blood sugar levels. According to the Centers for Disease Control and Prevention (CDC), following a balanced diet can help maintain consistent blood sugar levels and reduce the risk of hypoglycemia.
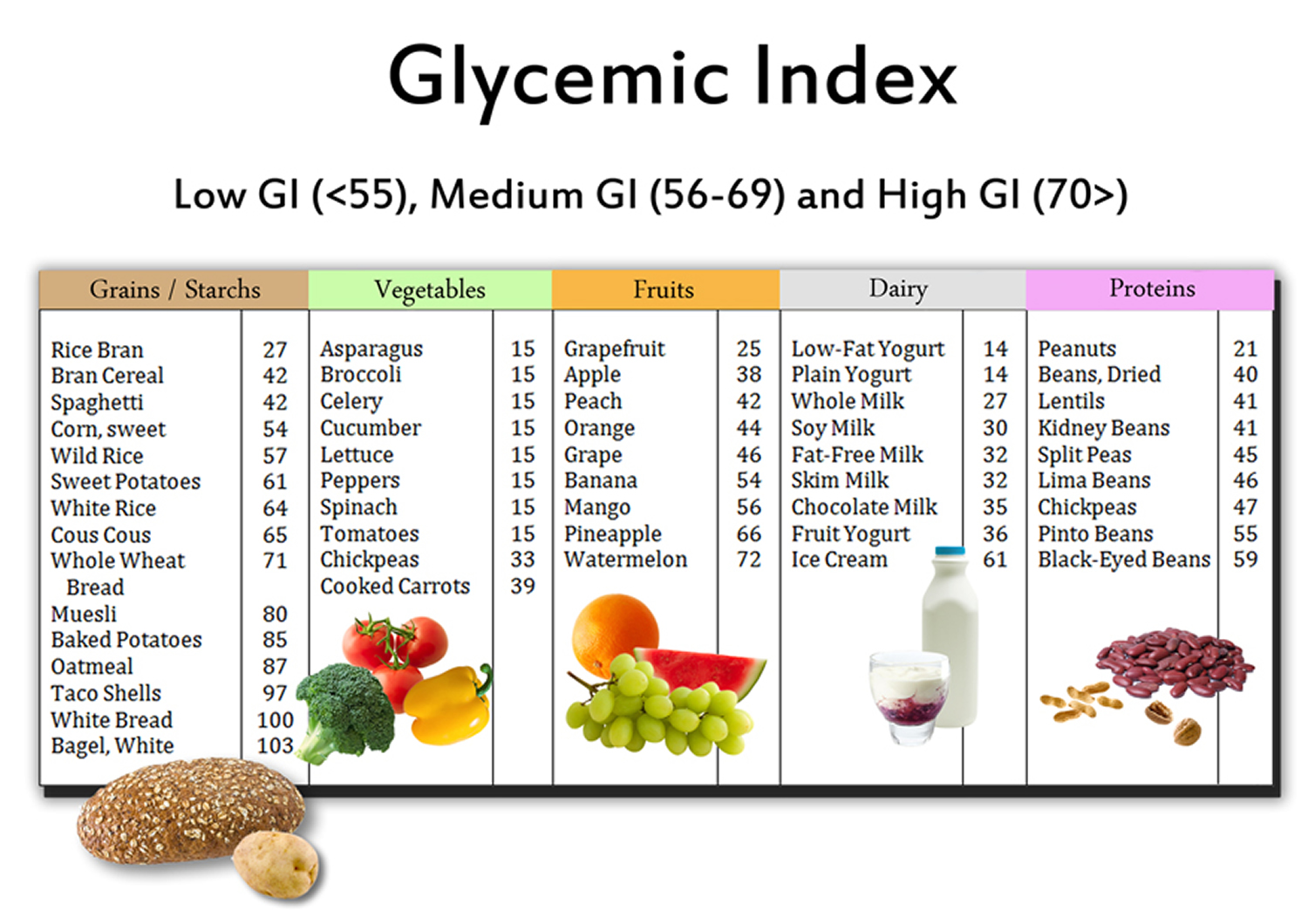
Recommended Food Types and Portion Sizes
Focus on incorporating whole grains, lean proteins, healthy fats, and plenty of fruits and vegetables into your diet. Portion control is equally important; overeating can lead to spikes in blood sugar. The National Institute of Diabetes and Digestive and Kidney Diseases provides a useful guide for portion sizes.
The Importance of Regular Meals and Snacks
Regular meals and snacks can help keep your blood sugar levels stable. Skipping meals or going too long without eating can cause your blood sugar to drop, leading to hypoglycemia. It’s recommended to eat every three to four hours.
Role of Medication in Managing Low Blood Sugar
Medications play a significant role in the management of hypoglycemia or low blood sugar. They help regulate the amount of glucose in the blood by either stimulating the pancreas to produce more insulin or helping the body use insulin more effectively. This helps prevent the onset of hypoglycemic symptoms and reduces the risk of complications.
Commonly Prescribed Medications
Commonly prescribed medications for hypoglycemia include Glucagon, Diazoxide, and Octreotide. Each has different mechanisms of action but all aim to increase blood glucose levels. It’s important to understand the specific medication you’re prescribed to effectively manage your condition.
How to Use Medication Safely and Effectively
Safe and effective use of medication involves adhering to prescribed dosage and timing, recognizing potential side effects, and regular monitoring of blood glucose levels. Always consult your healthcare provider for medication-related queries and never adjust your dosage without professional advice.
Exercise and Lifestyle Modifications for Managing Low Blood Sugar
Proactive management of your low blood sugar can start with a simple step – incorporating regular physical activity into your daily routine. The CDC reports that consistent exercise can help regulate blood glucose levels, along with warding off conditions like heart disease and obesity.
It’s vital to choose suitable forms of exercise, such as brisk walking, swimming, or cycling. These low-impact activities can help manage blood sugar levels without putting undue stress on your joints.
Lastly, lifestyle changes such as stress management can play a critical role. Chronic stress can cause blood sugar levels to spike, so techniques like meditation, deep-breathing exercises, or yoga can be beneficial.
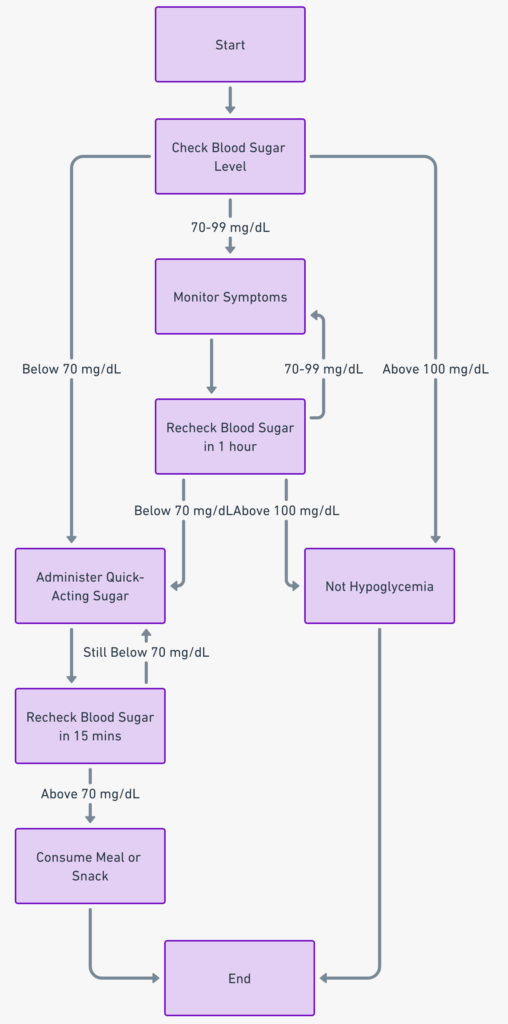
Recognizing a Hypoglycemic Emergency
Low blood sugar, or hypoglycemia, can come on unexpectedly, putting you at risk of a medical emergency. Key symptoms include sudden fatigue, shaking, sweating, blurred vision, and confusion. If you’re diabetic, regular monitoring of blood glucose levels is essential to detect hypoglycemia early.
Responding to a Hypoglycemic Episode
- Immediately consume 15-20 grams of fast-acting carbohydrates, like fruit juice or glucose tablets.
- Re-check your blood sugar levels after 15 minutes. If it’s still low, consume another 15 grams of carbohydrates.
- If symptoms persist or worsen, seek immediate medical attention.
Preparing an Emergency Response Plan
Plan ahead to manage hypoglycemic episodes effectively. Include details like emergency contacts, location of glucose sources, and steps for treating low blood sugar. Regularly update your plan and share it with family and friends. The Federal Emergency Management Agency offers resources to help you create a comprehensive plan.